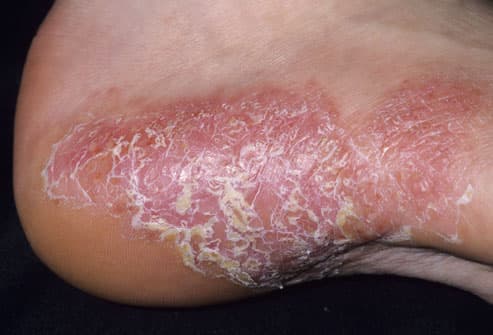
Lymphomatoid papulosis
Related Terms and Key Words: CD30+ lymphoma, eccrinotropic, granulomatous, lymphomatoid papulosis, methotrexate, lymphedema, papulonodular skin eruption, Primary cutaneous CD30 + lymphoproliferative disorder, Cutaneous T-cell lymphoma, Proliferative T-cell disorder, WHO/EORTC classification, chemokines, chemokine receptors
Definition:
A chronic skin disease that presents with characterists of malignant T-cell lymphoma. However, it is important to remember that lymphotoid papulosis (LyP) is not classified as a true lymphoma. Also, it does not spread and is not fatal. It is therefore described as histologically malignant, but clinically benign. (1)
It is classified as a lymphoproliferative disorder. These account for about 25% of cutaneous T-cell lymphomas. The condition occurs equally between men and women and usually occurs in the fifth decade. Clinically, black people appear to have the disease much less frequently then other races.
The term lymphomatoid papulosis originally was used by Macaulay[1] in 1968 to describe “a self-healing rhythmical paradoxical eruption, histologically malignant but clinically benign.” Due to the typical waxing and waning clinical course, lymphomatoid papulosis was previously considered a pseuodolymphomatous inflammatory process. However, the classification system for cutaneous lymphomas has evolved rapidly, and, during consensus meetings in 2003-2004, the World Health Organization—European Organization for Research and Treatment of Cancer (WHO-EORTC) classification grouped lymphomatoid papulosis among the indolent cutaneous T-cell lymphomas. (2)
LyP is divided into three subtypes, they include:
Type A - characterized by large CD30 atypical cells intermingled with a prominent inflammatory infiltrate. The large tumor cells have polymorphic convoluted nuclei with a minimum of 1 prominent nucleolus and resemble Reed-Sternberg cells when binucleate, as is seen in HD. Type A lymphomatoid papulosis is the most common histologic variant and accounts for 75% of all lymphomatoid papulosis specimens.
Type B is characterized by smaller (8-15 µm) atypical cells with hyperchromatic cerebriform nuclei resembling the atypical lymphocytes in MF. CD30+ large cells are rare, but epidermotropism is more common in this variant. There is some concern that Type B lymphomatoid papulosis may be better classified as a papular variant of MF.
Type C (diffuse large cell type) is characterized by sheets of CD30+ anaplastic large cells indistinguishable from ALCL, with the exception of the minimal subcutaneous invasion. These lesions resolve spontaneously and are therefore classified as lymphomatoid papulosis; however, some authorities view this histologic variant as borderline ALCL or, perhaps, pcALCL. (2)
Uncommonly, patients may have more than one histologic subtype of lymphomatoid papulosis or other recently described associated histologic patterns.
Risk Factors:
Unknown at the present time and there is debate on whether or not it may be genetically caused. Several genetic defect have been identified in LyP lesions, but the specific cause has not been identified.
A few investigators have also discovered viruslike particles in lymphomatoid papulosis lesions examined under electron microscopy.
Signs and Symptoms:
Lymphomatoid papulosis appears as recurrent small, raise skin lesions. The color ranges from red to brown in color. The most commonly occur on the trunk, arms, and legs in crops but may also occur on the palms, soles, face, and scalp. Very rarely, LyP lesions may be present in the mouth and throat. The lesions heal spontaneously within several weeks and leave a small, hypopigmented scar.
Diagnosis:
Done by skin biopsy. This is critical as the lesions may appear as the same for numerous other skin nodular growths.
Biopsies are also critical to rule out mycoses fungoides, cutaneous anaplastic large cell lymphoma, cutaneous Hodgkin’s disease, cutaneous leukemia, scabies, insect bites, and drug reactions.
If after biopsy the result come back other then lymphotoid papulosis, then the treating physician will order other types of tests to establish a correct diagnosis.
Differential Diagnosis
Cutaneous CD30+ (Ki-1) Anaplastic Large-Cell Lymphoma, Cutaneous T-Cell Lymphoma, Folliculitis, Insect Bites, Langerhans Cell Histiocytosis, Leukemia Cutis, Lymphocytoma Cutis, Milia, Miliaria, Scabies
Prognosis:
The disease itself is not fatal. However, 10 to 20% of patients will also develop an associated systemic lymphoma, typically anaplastic large cell, Hodgkinís disease, or mycoses fungoides.
If any type of secondary malignancy develops, then that would alter the outlook, depending on the type of malignancy.
Treatment:
Patients may choose not to treat the lesions and they usually heal spontaneously over 1-2 months.
Historically, treatment for the skin lesions themselves has been corticosteroid creams or ointment. Another option that can lead to faster healing is with low dose methotrexate. This is a type of chemotherapy that inhibits cell division. The one weak point in this treatment is that the lesions treated with methotrexate will generally return several weeks after therapy.
Another strong, aggressive treatment is oral psoralen plus ultraviolet light, so-called PUVA therapy.
Other treatments might include: carmustine, topical nitrogen mustard, topical MTX, topical imiquimod cream, intralesional interferon, low-dose cyclophosphamide, chlorambucil, medium-dose UVA-1 therapy, excimer laser therapy, photodynamic therapy, and dapsone help disease suppression.
Mortality/Morbidity
Lymphomatoid papulosis has a chronic, indolent course in most patients.
However, associated lymphomas may arise with LyP. These include immunoblastic lymphoma, lethal midline granuloma (currently considered as natural killer cell lymphoma in many patients), and systemic lymphocytic lymphoma. In most patients, the malignancy develops many years after the diagnosis of lymphomatoid papulosis.
see also:
 =
= 99) receiving systemic anticancer therapies and/or radiotherapy at Northwestern University. Subjects were assessed at the initial visit for adverse skin reactions based on the National Cancer Institute’s Common Terminology Criteria for Adverse Events version 3.0 and completed the Skindex-16 questionnaire, a self-reported dermatology-specific QoL instrument. All subjects were provided with three test articles and were instructed to use each test article once daily for 4 weeks. At the 4-week follow-up (n
99) receiving systemic anticancer therapies and/or radiotherapy at Northwestern University. Subjects were assessed at the initial visit for adverse skin reactions based on the National Cancer Institute’s Common Terminology Criteria for Adverse Events version 3.0 and completed the Skindex-16 questionnaire, a self-reported dermatology-specific QoL instrument. All subjects were provided with three test articles and were instructed to use each test article once daily for 4 weeks. At the 4-week follow-up (n =
= 77), the Skindex-16 was readministered, adverse skin reactions were assessed, and tolerability questionnaires were administered for each article used.
77), the Skindex-16 was readministered, adverse skin reactions were assessed, and tolerability questionnaires were administered for each article used.